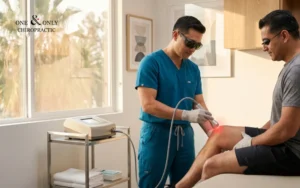
EMS vs. NMES/FES: What’s the Difference and When Are They Used?
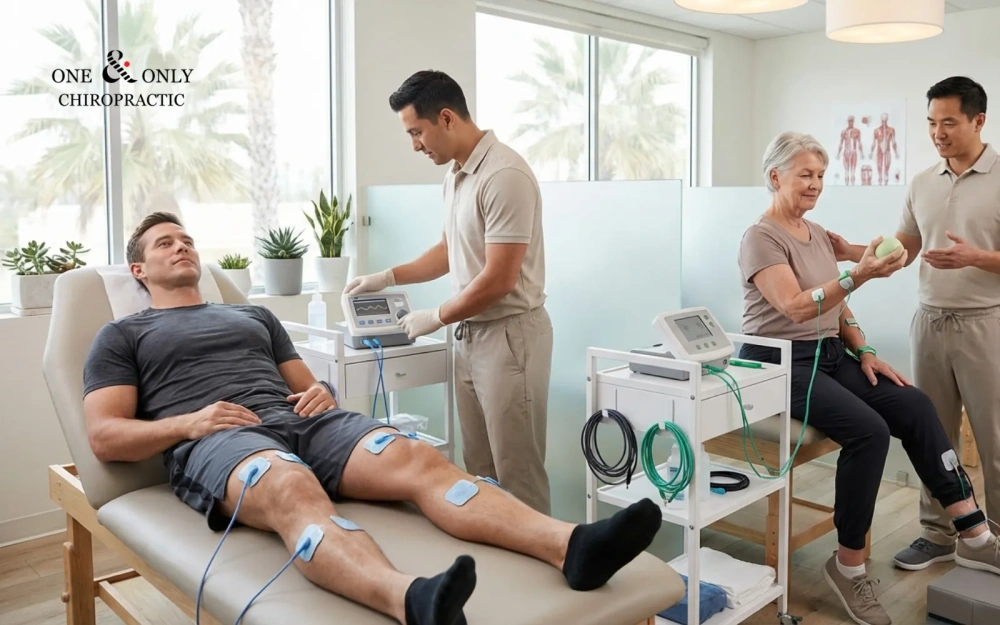
- What are EMS NMES and FES and how do they differ?
- How does electrical muscle stimulation work?
- What is neuromuscular electrical stimulation and when is it used?
- What is functional electrical stimulation and when is it used?
- What are the differences between EMS and NMES that matter for patients?
- How do NMES and FES compare for movement and gait training?
- Who is a good candidate and who should avoid these therapies?
- What does the scientific evidence say about outcomes?
- How are these therapies used in chiropractic and physical therapy care plans in Santa Ana California?
- What should you expect during a session and how should you prepare?
- How do home units compare with clinic grade devices and what is safe?
- What do insurance and California regulations say about these modalities?
- How can you decide between EMS NMES and FES for your goals?
- Who is One and Only Chiropractic in Santa Ana California and how can we help you take next steps?
- Where can you find the sources referenced in this article?
What are EMS NMES and FES and how do they differ?
If you are comparing EMS vs NMES FES, you are not alone. These acronyms describe related but distinct ways of using electrical currents on the surface of the skin to activate nerves and muscles. Understanding the differences helps you choose an approach that matches your goals, whether that is muscle recovery after exercise, muscle re education after injury, or help with walking after a neurological condition.
Electrical muscle stimulation often called EMS typically targets healthy peripheral nerves to create visible muscle contractions for training or recovery. Neuromuscular electrical stimulation called NMES is closely related but is used to strengthen weak or inhibited muscles and to retrain coordinated activation as part of rehabilitation. Functional electrical stimulation known as FES is a form of NMES applied during a task like walking or reaching so the stimulation assists a specific movement such as lifting the foot to clear the ground during gait. All of these devices are regulated medical devices in the United States and most fall under the powered muscle stimulator classification overseen by the Food and Drug Administration [1]. Consumer oriented devices are also subject to FDA regulation and marketing rules that emphasize safety and appropriate claims [11].
Each method has a place. EMS may be used to promote circulation or reduce exercise related soreness. NMES is commonly integrated with strengthening and mobility work to address weakness or neuromuscular inhibition after surgery or injury. FES is widely used in neurologic rehabilitation to support functional tasks such as gait training in stroke and other central nervous system conditions [4]. Later sections explain how these approaches work, who may benefit, and what to consider in Santa Ana California when adding them to your care plan.

How does electrical muscle stimulation work?
Electrical muscle stimulation uses controlled pulses delivered through surface electrodes to depolarize motor nerves that innervate a muscle. When the nerve fires, the muscle contracts. Clinicians and trained users can adjust parameters such as pulse width, frequency, and intensity to shape the contraction. For example, lower frequencies can produce gentle twitches while higher frequencies can create a tetanic contraction that looks and feels like steady muscle tension [7].
Why do people use EMS for recovery and training? Many choose EMS to supplement workouts, to recruit additional muscle fibers, or to promote blood flow after intense sessions. Some prefer it when traditional exercise is limited by joint irritation or when a targeted area needs light loading without joint compression. It is important to keep expectations realistic. The FDA cautions consumers not to rely on EMS alone for performance or cosmetic goals and to understand that these devices are regulated for specific indications [11]. In a clinical setting, EMS style stimulation may also be used for pain modulation or muscle spasm reduction when indicated, often as part of a broader plan that includes manual therapy and active exercise [6].
Key takeaways for EMS include the following practical points:
- What it targets EMS targets intact peripheral motor nerves to create visible muscle contractions.
- When to consider it Consider EMS for muscle conditioning, circulation support, or when you want a gentle adjunct to training or recovery days.
- What it does not replace-strong> EMS does not replace progressive resistance training, movement skill practice, or nutrition.
What is neuromuscular electrical stimulation and when is it used?
Neuromuscular electrical stimulation is used to strengthen weak or inhibited muscles and to improve timing and coordination. After injury, surgery, or periods of immobilization, the brain and spinal cord can reduce drive to a muscle, and the muscle itself can atrophy. NMES helps by artificially activating the motor nerve to produce a contraction while you practice voluntary effort. Over time, this pairing can improve motor unit recruitment and restore function as part of a structured plan of care [7].
Common reasons to choose NMES for rehabilitation include quadriceps inhibition after knee surgery, gluteal weakness related to hip or low back issues, and shoulder stabilizer weakness after rotator cuff procedures. In the early phases of post surgical rehab when heavy loads are not allowed, NMES can provide a meaningful training stimulus while respecting tissue healing timelines. Later, it can intensify targeted activation during functional exercises such as sit to stand, step ups, and reaching patterns [6].
Evidence reviews describe how NMES parameters influence outcomes. For strength and hypertrophy, moderate to high intensities that create a robust yet safe contraction are typically used. For re education, synchronizing the stimulation with the start of the voluntary effort encourages the nervous system to relearn timing. Importantly, NMES works best when combined with progressive exercise that advances as tolerance and tissue healing allow [7].
What is functional electrical stimulation and when is it used?
Functional electrical stimulation applies stimulation during a purposeful task to help complete the movement. A classic example is ankle dorsiflexion during walking to prevent toe drag known as foot drop. With FES, a sensor or switch triggers stimulation to the peroneal nerve or anterior leg muscles during the swing phase of gait. This assists foot clearance and can reduce trips while also providing practice that may carry over to voluntary control [4]. In neurologic rehabilitation, FES can also support reaching and grasping, cycling, or sit to stand practice, depending on the system used and the goals of care [8].
Why does FES matter in our community. Stroke remains a leading cause of serious long term disability in the United States, with nearly 800 thousand people affected each year [3]. Foot drop after stroke or other central nervous system conditions can significantly limit safe community ambulation. Clinical guidance from national bodies in the United Kingdom and expert resources in the United States support the use of FES for carefully selected individuals with foot drop of central origin when delivered by trained clinicians as part of a comprehensive program [4][8].
What are the differences between EMS and NMES that matter for patients?
If you are weighing EMS vs NMES, a few differences stand out that can help you decide which approach aligns with your situation.
- Primary goal EMS is often used for general conditioning or recovery. NMES is designed for rehabilitation, muscle re education, and strength restoration after injury or surgery [6].
- Typical users EMS may be used by healthy athletes or fitness enthusiasts. NMES is typically used under the guidance of licensed clinicians for patients with weakness, inhibition, or motor control deficits.
- Timing with movement EMS can be used at rest or during light movement. NMES is commonly paired with specific therapeutic exercises to improve activation at the right time and intensity.
- Regulatory pathway Both EMS and NMES devices are generally considered powered muscle stimulators that in most cases require FDA premarket notification known as 510 k, which reviews substantial equivalence to legally marketed devices [1][2].
- Clinical oversight NMES is typically dosed and progressed in a plan of care. EMS used for recovery may be self directed but should follow device labeling and safety guidance, especially for people with medical conditions [11].
When comparing EMS vs FES, keep in mind that EMS is not task specific by design, while FES always aims to assist a task such as lifting the foot during walking. Likewise, when thinking about NMES vs FES, both can strengthen nerves and muscles, but FES is synchronized to a function and often relies on sensors, switches, or programmed timing to deliver current at the exact moment you need help [4][8].
How do NMES and FES compare for movement and gait training?
NMES and FES both recruit motor units that may not be easily activated voluntarily after injury or neurologic conditions. The difference is context. NMES focuses on strengthening and activation quality during drills. FES provides real time assistance during a task. For gait training, NMES might be used to strengthen ankle dorsiflexors and plantarflexors with seated or standing exercises. FES would then be used while walking to lift the foot during swing or to assist knee control during stance, often with a foot switch or tilt sensor to time the current to the gait cycle [4][8].
In clinic practice, many patients progress from isolated NMES strengthening to FES assisted walking, then to unassisted walking as carryover improves. The decision to use NMES, FES, or a blend depends on diagnosis, timing after injury, spasticity levels, skin tolerance, and goals that matter to you such as safer sidewalk walking in Santa Ana or improved endurance on local trails.
Who is a good candidate and who should avoid these therapies?
Appropriate screening and dosing help keep electrical stimulation safe and effective. Your clinician will review your medical history, skin condition, and functional goals to determine fit. While device labeling varies, common indications and contraindications include the following general themes, with clinical judgment guiding final decisions.
- Who may benefit People with muscle weakness after injury or surgery, individuals with neurologic conditions who have task specific deficits such as foot drop, and athletes who want a gentle adjunct on recovery days may benefit when programs are tailored and supervised [6][8].
- Who should avoid or seek medical clearance People with implanted pacemakers or defibrillators, active infections at the electrode site, areas of impaired sensation, known or suspected deep vein thrombosis, or active malignancy in the treatment area generally should not receive stimulation at those locations. Pregnancy is a common precaution, especially avoiding abdominal or lumbar regions. Always follow device labeling and consult your physician if you have questions about medical conditions [6][11].
- Where not to place electrodes Avoid anterior neck over the carotid sinus and do not place electrodes where they might cause current to pass through the chest in a way that could interact with cardiac rhythm devices [11].
This is educational information and not a substitute for an evaluation. If you are considering stimulation and have a complex medical history, reach out to your healthcare team for clearance and individual guidance.
What does the scientific evidence say about outcomes?
Research over several decades has explored how neuromuscular electrical stimulation affects muscle strength, motor control, and function. Reviews of NMES describe meaningful improvements in muscle strength and activation when sufficient intensity is used and when patients combine stimulation with progressive exercise and task practice [7]. Methodological factors such as electrode placement, pulse duration, and session frequency influence outcomes. Across protocols, consistency and gradual progression remain essential.
For FES, published guidance and clinical research support its role in gait training for selected individuals with central neurologic conditions who have foot drop. Guidance from the National Institute for Health and Care Excellence indicates that FES for foot drop of central origin can be used with normal arrangements for clinical governance, consent, and audit, which means it can be offered in routine practice by trained teams who monitor outcomes and safety [4]. Expert resources in physical medicine and rehabilitation detail additional applications such as upper limb function and cycling in spinal cord injury with careful screening and parameter selection [8].
Stroke remains a key context for FES research and implementation. With nearly 800 thousand strokes per year in the United States, even small gains in walking speed and safety can have meaningful community impact and quality of life benefits [3]. Studies have reported improvements in foot clearance, walking speed, and user satisfaction with FES systems compared with traditional bracing in selected cases, while noting that individual responses vary and that practice plus progression are central to lasting gains [4][8].
For EMS used in recovery, authoritative sources emphasize using these devices as an adjunct to training rather than a replacement. The FDA has issued consumer updates clarifying that marketing claims must be supported by evidence and that users should follow instructions to avoid skin irritation or improper use [11]. In all cases, consistent, supervised use that is integrated into a plan of care is more likely to deliver benefits than occasional, unsupervised sessions.
How are these therapies used in chiropractic and physical therapy care plans in Santa Ana California?
In Santa Ana and across California, chiropractic and physical therapy teams often work together to help patients return to activity. Electrical stimulation is one of several physical therapy modalities that can support recovery when used thoughtfully. In a chiropractic setting, stimulation may be paired with manual therapy, joint mobilization, and corrective exercise. If your plan includes neuromuscular electrical stimulation, your team will likely use it to improve activation of specific muscles during targeted drills, then advance to functional tasks as you progress. If your needs include foot drop or other task specific deficits, functional electrical stimulation for gait training may be considered where appropriate and available [6][8].
California regulations recognize physiotherapy as part of chiropractic practice when delivered within scope and according to board rules. The Board of Chiropractic Examiners provides current regulations and scope details for licensed chiropractors practicing in the state, including Santa Ana [9]. Your care team will follow device labeling, document indications, and obtain consent before adding any modality to your plan.
Plans are always individualized. For example, a post surgical rehab plan for a knee may begin with gentle NMES to the quadriceps along with range of motion and swelling control, then progress to closed chain strengthening, dynamic balance, and return to running. For a patient recovering from a neurologic event with persistent foot drop, a plan may include trials of FES for community walking, caregiver training, and home exercise that emphasizes practice and safety.
What should you expect during a session and how should you prepare?
Most sessions begin with a brief check in about your goals, skin condition, and recent changes in health. Your clinician will clean the skin and place electrodes over the target muscle bellies or near the motor points. They will then set parameters and gradually increase intensity to a safe and tolerable level. You will usually be asked to try to contract the muscle at the same time the current is delivered, especially during NMES, to encourage carryover. During FES for gait training, sensors or switches help time the current to your walking pattern.
To prepare, consider the following tips:

- Wear accessible clothing Shorts for knee work or loose sleeves for shoulder sessions make electrode placement easier.
- Avoid lotions on the treatment area Lotions can reduce electrode adhesion and change skin impedance.
- Report skin sensitivity or allergies-strong> Let your clinician know about reactions to adhesives or gels so they can adjust materials.
- Share updates about your health Tell your team about new diagnoses, procedures, or implanted devices before stimulation sessions.
- Expect progressive dosing Intensity, on off timing, and session length will progress as you adapt and as tissues heal.
Discomfort should stay within a tolerable range, and the skin should be checked after sessions. Mild redness under electrodes that resolves within an hour is common. Persistent redness, blistering, or unusual pain should be reported immediately so your team can modify the approach.
How do home units compare with clinic grade devices and what is safe?
Home electrical stimulators range from consumer EMS units to prescription NMES and FES systems. Clinic grade devices used by licensed professionals often have broader parameter ranges, stronger output, and features that support task specific training. Home use can be effective and convenient when the device is appropriate for your condition, parameters are set correctly, and you have clear safety instructions.
Consider the following when thinking about home use:
- Device type and indication Make sure the device type matches your goals. EMS for general conditioning differs from NMES for rehab and from FES for gait training. The labeling should clearly state intended use and contraindications [1][11].
- Regulatory status In the United States, most powered muscle stimulators are class II devices that go through the FDA 510 k pathway. Ask your provider about the device clearance and whether a prescription is required [1][2].
- Training and follow up Proper electrode placement, parameter selection, and skin care reduce risks and improve outcomes. Plan for an initial teaching visit and follow up checks with your clinician.
- Safety first Follow instructions, avoid prohibited areas, and stop if you notice irritation or unexpected pain. Contact your clinician with any concerns [6][11].
What do insurance and California regulations say about these modalities?
Coverage varies by plan and by diagnosis. Some plans cover NMES or FES when medically necessary for conditions such as post surgical weakness or foot drop of central origin. Others may classify EMS for general conditioning as non covered. Because policies differ, the most reliable path is to contact your insurer with your specific diagnosis and the device code your clinician intends to use. Your care team can provide documentation that explains the medical necessity of the modality within your plan of care. No coverage outcomes can be guaranteed because each plan has distinct terms and prior authorization requirements.
In California, chiropractors are licensed by the Board of Chiropractic Examiners. The board regulations and scope information describe the use of physiotherapy within chiropractic practice when delivered in compliance with state law and board rules. Providers in Santa Ana follow these regulations, maintain current licenses, and document informed consent and indications for any modality including electrical stimulation [9]. When electrical stimulation is part of care in an interprofessional plan, providers also coordinate with prescribing physicians and physical therapists as needed to ensure appropriate continuity of care.
How can you decide between EMS NMES and FES for your goals?
Choosing among EMS, NMES, and FES starts with clarifying your primary goals, your medical history, and your current phase of recovery or training. These questions can help you and your clinician decide what fits best.
- Is your goal general recovery or targeted rehabilitation EMS for recovery may help with gentle conditioning and comfort. NMES for rehabilitation is better suited to address specific weakness or inhibition after injury. FES is reserved for task assistance like gait training when timing support is needed [4][6].
- Do you have neurologic deficits that limit tasks If foot drop or hand opening is limiting function, an FES trial may be considered by your rehab team where appropriate and available [4][8].
- What are your safety considerations Any history of implanted cardiac devices, skin conditions, or other medical issues should be reviewed before using stimulation. Clearance may be needed in some cases [11].
- How will the modality integrate with a full plan The best outcomes come when stimulation supports a larger program that includes progressive exercise, mobility work, and education tailored to your goals [7].
If you are in Santa Ana California and wondering how to apply this in real life, start with an evaluation. A qualified clinician can test strength, movement, and task performance, then recommend the right blend of manual therapy, exercise, and if appropriate, electrical stimulation to help you move forward safely.
Who is One and Only Chiropractic in Santa Ana California and how can we help you take next steps?
At One and Only Chiropractic we help people in Santa Ana make informed choices about care, including when to use electrical stimulation and how to get real world results. Our wellness and injury clinic focuses on evidence based, minimally invasive approaches that combine education, hands on treatment, and movement training for patients of all ages. When appropriate, we integrate chiropractic electrical stimulation within broader plans that may also include soft tissue care and corrective exercise. If you are comparing EMS vs NMES or wondering if FES for gait training could help, our team will walk you through the options in plain language and with realistic expectations.
Here is how we support your decision making and outcomes:
- Clear evaluation and goal setting We begin with a thorough history and movement assessment so the plan matches your goals whether that is pain management, post surgical rehab, return to sport, or safer community walking.
- Integrated modalities and exercise-strong> When indicated, we use neuromuscular electrical stimulation during targeted drills to improve activation, then build on that with progressive strength and mobility work. For neurologic needs, we can coordinate FES trials for gait training with our trusted local partners.
- Education that empowers you We explain indications and contraindications, home safety, and how to track progress so you know exactly why a modality is being used and what to expect at each step.
- Personalized progression Parameters and exercises are advanced in small, safe steps so the program stays challenging without overwhelming healing tissues.
- Collaboration across disciplines We collaborate with physical therapy and medical providers when a team approach will improve continuity and outcomes for you.
- Local access and support Our Santa Ana location makes it easier to fit care into your week. We share practical strategies for getting walks in nearby neighborhoods and parks as endurance improves.
- Experienced clinicians Our team brings years of combined experience with musculoskeletal and neurologic conditions, including athletes, workers, students, and older adults.
- Real stories and results Patients commonly report clearer muscle activation and confidence returning to activities as plans progress. While individual results vary, consistent practice and supportive coaching make a difference.
- Easy next steps If you are ready for an evaluation or simply want to ask questions about EMS, NMES, or FES, call us at 949 800 8525. We are here to help you choose a safe and sensible path forward.
We operate in Santa Ana California and serve surrounding communities. Our approach is patient centered and education forward. We do not make guarantees about outcomes. Instead, we focus on clear planning, careful dosing, and steady progress that reflects your goals and current health status.
Where can you find the sources referenced in this article?
- Powered Muscle Stimulator 21 CFR 890.5850 – eCFR
- Premarket Notification 510 k – FDA
- Stroke Facts – Centers for Disease Control and Prevention
- Functional electrical stimulation for drop foot of central neurological origin – NICE
- Foot Drop – National Institute of Neurological Disorders and Stroke
- Electrical Stimulation Guide – American Physical Therapy Association
- Physiological and methodological considerations for NMES training – PubMed
- Functional Electrical Stimulation – AAPM and R KnowledgeNow
- Regulations and Scope of Practice – California Board of Chiropractic Examiners
- Stroke Rehabilitation – MedlinePlus
- What to know about electrical muscle stimulation devices – FDA Consumer Update
- Stroke Rehabilitation Information – NINDS